P. ZAMBONI, M. G. MARCELLINO, M. CAPPELLI, C.
V. FEO, V. BRESADOLA, G. VASQUEZ. A. LIBONI
Objective. Evaluation of saphenous vein sparing surgical
procedures alternative to high ligation and distal stab avulsion, in terms
of effectiveness and suit-ability for eventual bypass
surgery.
Experimental design. Prospective evaluation of 421
operations for primary varicose veins, 64 external valve-plasties of the
sapheno-femoral junction (EV-SFJ), (42 performed using the hand sewing
technique and 22 using the Veno-cuff device), mean follow-up 52 months,
and 357 hemodynamic correction of varicose veins (French acronymis CHIVA),
mean follow-up 49 months. Moreover, a subgroup of 27 patients was operated
on using the CHIVA technique in two steps, mean follow-up 18
months.
Setting. Institute of General Surgery, University of
Ferrara. Institutional practice, one-day surgery.
Patients.
Patients were selected using clinical and duplex scanning evaluations, and
classified according to CEAP criteria. Patients with varicose veins due to
sapheno-femoral reflux with duplex scanning evidence of mobile valve
leaflets underwent EV-SFJ. The other patients were operated on using the
hemodynamic correction technique. Interventions. EV-SFJ restores valve
function correcting vein wall dilatation by applying an external
prosthesis. CHIVA consists of selected ligatures of the superficial veins
that allow superficial blood aspiration in the deep veins through the
perforators as well as the preservation of saphenous
drainage.
Measures. The outcome was evaluated with independent
clinical and ultrasonographic examinations; pre and postoperative AVP and
LRR-RT measurements were assessed in 125 cases. Data from self-assessment
of the functional and cosmetic result of the patients of the CHIVA group
were also obtained using a scoring system. Moreover, scanning the
preserved long saphenous vein the rate of long saphenous vein suitable as
arterial conduit following sparing surgery was also
evaluated.
Results. Overall long saphenous vein patency
registered after EV-SFJ and CHIVA was 94%. Varicose veins recurrence rate
was 12% and 11%, respectively. Postoperative AVP and LRR-RT improvement
was stas-tically significant (p<0.001).
Conclusions. These
two alternative procedures seem to be effective In varices treatment
following the proposed indications and techniques. In addition, they
appear able to preserve a more significant rate of saphenous veins
suitable for eventual bypass surgery than high ligation and multiple
cosmetic avulsion.
Saphenous vein sparing surgery for varicose vein disease is still
controversial in the literature. Many groups note the increased risk of
varicose vein recurrence if the long saphenous vein is not excised at the
time of initial surgery. On the other hand, some comparative studies show
no significant differences in recurrence rate between stripped and
non-stripped limbs, especially if the preoperative assessment allows
mapping of the insufficient veins. Alternative long saphenous vein sparing
surgical procedures such as the external valve-plasty of the
sapheno-femoral junction (EV-SFJ) and the hemo-dynamic correction of
varices (French acronym is CHIVA), seem to be effective for varicose
treatment and, maintaining a high saphenous vein patency rate more useful
for future grafting as compared to high ligation and distal stab avulsion.
This paper shows a prospective long-term evaluation of these treatments
defining precisely the patients' population by means of CEAP
classification and ultrasonographic criteria: moreover, the rate of long
saphenous vein suitable as an arterial conduit following these new
procedures is evaluated by means of duplex, scanning the preserved vein.
Materials and methods
Four hundred and twency-one cases of primary varicose veins disease
with epical sapheno-femoral reflux have been selected for alternative
saphenous vein sparing surgery at the Vascular Laboratory of our
Institute.
EV-SFJ
Patients' selection and preoperative assessment.-64 patients (15 men,
49 women, 20-70 years old. mean age 41 years old, were selected for EV-SFJ
using the following criteria:
Clinical.-Primary varices, symptoms of venous insufficiency,
absence of prior thrombophlebites or sclerotherapy.
Duplex scanning (Ansaldo AU 530, 7.5-10 MHz probe,
Italy).-Evidence of mobile valve leaflets of uniform length at the
sapheno-femoral junction (SFJ). Sapheno-femoral reflux and competence of
the deep venous system. Long saphenous vein (LSV) diameter at the mid
thigh was measured both preoperatively and 6 months later.
CEAP classification.-52 patients were retrospectively and 12
prospectively classified according to the new CEAP classification
criteria. Regarding the clinical class, C, all the patients were
symptomatic and affected by simple varicose veins without oedema, skin
changes and/or ulcerations. The etiology, E, was always primary. The
anatomical distribution of cases, A, was in the LSV above the knee in 27
cases, above and below the knee in 35. Perforators were found to be
incompetent at the thigh in 34 cases and at the calf in 42. Finally the
pathophysiology of the disease, P, was due to reflux in all cases. The
following algorithm describes the selected patients: C2s, Ep, As2-3 p
17-18. Pr.
Venous function assessment.-32 patients underwent preoperatively
and 6 months postoperatively ambulatory venous pressure (AVP) and light
reflection rheography-refilling time (LRR-RT) measurements.
 |
Fig 1-Left: Private Circulation with the
hemodynamic pattern of type 1 Shunt (outlet of the re-entry
perforator on the LSV). Right: Procedure performed in such cases: 1)
High ligation, 2) Disconnection from the LSV of the varicose
tributary and, eventually, avulsion with cosmetic incisions. Legend:
LSV. long saphe-nous vein: SSV short saphenous vein: DV, deep venous
system: Giac, Giacomini vein: TV, tributary. PV, perforator. Arrows,
blood flow direction determined by Doppler mode.
|
 |
Fig. 2.-Left: Private Circulation with
the hemodynamic pattern of type III Shunt (outlet of the re-entry
perforator on a tributary of the LSV, type III Shunt with re-entry
in Table III). Right: Procedure performed in such cases: 1) High
ligation. 2) Interruption of the superficial vein just below the
outlet of the insufficient perforator. Legend: see Figure 1.
|
 |
Fig. 3.-Left: Private Circulation with
the hemodynamic pattern ot type III Shunt (outlet of the re-entry
perforator on a tributary of the LSV). Right: Procedure performed in
such cases (type III Shunt without reentry in Table III): 1) High
ligation. 2) Disconnection from the LSV and avulsion with cosmetic
incisions of the varicose tributary. |
 |
Fig 4-Left: Private Circulalion with the
hemodynamic pattern of type III Shunt "short and/or deep" (re-entry
perforator on a tributary close to the origin from the LSV (short)
or deep, and thus not visible). Right: Procedure performed in such
cases: 1) High ligation. 2) Interruption of the superficial vein
just below the outlet of the insufficient perforator, and eventual
cosmetic phlebeciomy below this point. Legend: see Figure 1.
|
 |
Fig. 5.-Left: Private Circulation with
the hemodynamic pattern of type III Shunt (outlet of the re-entry
perforator on a tributary of the LSV) and Doppier signal recorded on
the saphenous trunk under squeezing manoeuver performed in standing:
a forward flow of the saphenous vein during muscular contraction is
followed by a reverse flow during muscular relaxation. Right:
Procedure performed according to the treatment named CHIVA in two
steps: 1) First step, disconnection from the LSV and eventual
avulsion with cosmetic incisions of the varicose tributary Doppler
trace demonstrates under squeezing manoeuver performed in standing a
forward flow of the saphenous vein during muscular contraction and
the disappearance of the reverse flow during muscular relaxation.
Legend: see Figure 1. |
 |
Fig. 6.-Left: Private Circulation with
the hemodynamic pattern of typeI Shunt (outlet of the re-entry
perforator on the LSV with a secondary reflux from an incompetent PV
proximal to the re-eniry PV). Right: Procedure performed in such
cases: 1) High ligation. 2) Interruption of the superficial vein
just below the outlet of the insufficient perforator. The ligature
transforms a secondary reflux point into a re-entry point, with a
Doppler detectable inward flow, and preserves at least two LSV
segments. Legend see Figure 1. |
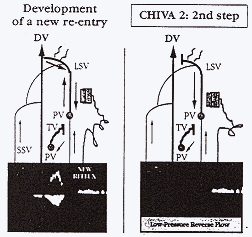 |
Fig. 7.-Left: After development of a new
re-entry perforator, Doppler signal of reflux is newly recorded on
the saphenous trunk. Right: Second step of the procedure is high
ligation that determines a low-pressure reverse flow toward the
re-entry perforator. Legend: see Figure 1.
|
Operations.-Under local anaesthesia, the saplieno-femoral
junction was exposed and the terminal valve encircled by an external
prosthesis, using the hand-sewn technique previously reported. In 42 cases
the valve-plasly was performed using a PTFEe sleeve (Gore-Tex, USA) 0.4 mm
thick. 1-1.5 cm long to surround an average circumference of 1.7 cm. The
graft was fixed around the vein with a 7/0 PTFEe interrupted suture. In 22
cases the valve- plasly was performed using the Veno-cuff device (Vaso
Inc., USA) surrounding the valve site with a Dacron reinforced silicone
cuff.
Optimal circumference for valve function restoration was
considered that of the saphenous vein below the valve, previously measured
in quiet standing by means of B-mode high resolution. Such a value was
selected by moving the calibrator and the cuff secured firing a stainless
steel surgical staples. When the terminal valve was absent or the sub
terminal was also very dilated, we performed a second valve-plasty of the
sub-terminal, too. This occurred in 41 cases (37 PTFEe sleeves and 4
Veno-Cuff). Patients were discharged 3-5 hours after surgery with
postoperative elastic stockings.
Intraoperative valve competence tests.-Intraoperative detection
of the restored valve function was made:
1. In all the treated cases
intraoperative C.W. Doppier examination (Stereodop 448 S, Echomed, 4-8 MHz
probe, France): The Valsalva and proximal compressive manoeuvres
demonstrated disappearance of reflux. Conversely, compressive distal
manoeuvres were used to detect LSV patency.
2. In 21 cases
intraoperative video angioscopic assessment was used.
CHIVA
Patients' selection and preoperative assessment.-Other 357 patients
with primary varicose veins syndrome with typical sapheno-femoral reflux
were treated by hemodynamic correction, using the following selection
criteria:
Clinical.-Primary and symptomatic chronic venous insufficiency
(CVI) of all clinical classes, absence of prior chrombophlebites and/or
surgical and sclerotherapic treatment.
Duplex scanning (Ansaldo AU 530. 7.5-10 MHz probe.
Italy).-Preoperative duplex detected patients with typical sapheno-femoral
reflux. excluding patients affected by varicose veins fed by different
primary reflux points. In addition duplex made it possible to outline on
the skin the points where the superficial veins should be interrupted (see
Preoperative duplex mapping). The LSV diameter at mid thigh was measured
boch preoperatively and 6 months later.
CEAP classification.-188 patients were retrospectively and 169
prospectively classified according to the new CEAP classification
criteria. The clinical class. C, ranged from C2 to C6 (267 with simple
varicose veins (C2), 60 with oedema (C3). 11 wich lipodermatosclerosis
and/or other skin changes (C4). 16 with healed (C5) and 3 with active
ulcer (C6): all the selected patients presented with classic symptoms of
CVI. of different severity. The etiology was, obviously, primary. The
anatomical distribution of cases was in the LSV above the knee in 104
cases, above and below the knee in 253 cases, perforators were found to be
incompetent at the thigh in 134 cases and at the leg in 283.. Finally the
pathophysiology was due to reflux in all cases. The following algorithm
describes the selected patients C2-6. EP. As2-3, p 17-18, Pr.
Venous function assessment.-73 patients underwent preoperacively
and 6 months postoperatively AVT and LRR-RT measurements.
Preoperative duplex mapping.-A preoperative skin map was
obtained by duplex in order to identifv the points where the superficial
veins had to be interrupted.
The ultrasonographic image of the
so-called "saphenous eye" is a precise and constant marker clearly
demonstrable in the transverse duplex access of the internal surface of
both the thigh and leg. This finding is typical of few superficial veins
and precisely, of the long. short and anterior saphenous and Giacomini's
vein. The image is due co the duplication of the superficial fascia around
the saphenous vein.
In all the selected patients duplex examination
allowed us to recognize and differentiate the saphenous vein from Other
superficial veins, as well as to identify the so-called Private
Circulation (PC) or Shunt, a vicious circle of blood between the
superficial and the deep veins in primary cases. The circle starts during
muscular relaxation, when the blood from the more proximal reflux point,
the SFJ, through the LSV and/or the superficial veins, flows downwards to
the re-entry point represented by a Perforating Vein (PV). and then into
the deep veins. The circle ends during the following muscular contraction,
when the blood flows forward through the deep veins, and then again to the
proximal reflux point when muscular relaxation occurs (Figs. 1. 2). Shunts
in varicose veins were classified in four types according to the CHIVA
theory. When the sapheno-femoral junction is incompetent, as in all the
selected patients, two models of private circulation (PC) have been
described: Type I Shunt and Type III Shunt. One hundred and eighty-six of
the selected patients (53%) showed the hemodynamic pattern of Type I
Shunt, in which the superficial branch of the PC, from the reflux point to
the re-entry point. is entirely represented by the LSV. and the re-entry
PV, obviously dilated, is situated on the LSV itself. In Figure I are
shown the points of surgical interruption in case of Type I Shunt
presentation. In contrast, 171 patients (47%) showed the hemodynamic
pattern of Type III Shunt, in which the superficial branch of the PC. from
the reflux point to the re-entry point, is represented either by the LSV
or by a TV of the LSV. In such cases the reentry PV is situated on the TV
instead of the LSV (Fig. 2).
Obviously, also the patients of this
group showed a proximal reflux point, the SFJ. and a secondary reflux
points at the outlet of incompetent TVs. one of which contains the outlet
of the re-entry PV. In Figures 2, 3, 4, 5 are shown examples of
hemodynamic presentations of Type III Shunt.
Operations.-All operations were performed under local
anaesthesia. The SFJ was exposed in the usual way, maintaining the
tributaries. The SFJ was clipped or disconnected (flush ligation). The
preserved tributaries allow the superficial and pelvic venous systems to
drain into the LSV, where the blood flow will be reversed toward the
re-entry perforators. In Type I Shunt, we ligated all the incompetent TVs
from their origin on the LSV. If the TV is particurarly dilated cosmetic
avulsion of its proximal tract can be performed, while the PV on the LSV
main trunk allows blood re-entry into the deep veins without
sapheno-femoral reflux overload. Moreover, in Type I Shunt a secondary
reflux from an incompetent PV proximal to the re-entry PV was detected in
31 cases (9% of the operated cases). (Fig. 6). In such a case we
interrupted the LSV just below the origin of the proximal PV. The ligature
transforms a secondary reflux point into a re-entry point, with a Doppler
detectable inward flow and preserves at least two LSV segments (Fig. 6).
In contrast, in Type III Shunt, the original technique proposed by
Franceschi in 1988, the so-called "CHIVA 1", consists of disconnecting
either the SFJ (the proximal reflux point) and all the incompetent TVs
from the LSV (the secondary reflux points), except chat containing the
re-entry PV (Fig. 2). Such a lactic allows us to maintain the LSV patency
and the drainage function, and was attempted in 72 cases (20% of ehe
operated cases); in addition the TV was ligated just below the outlet of
the re-entry PV (Fig. 2).
Thirty-five patients were operated on in the
same way but presented with the segment of the TV, which contains the
re-entry PV, close to the origin from the LSV (short) or deep, and thus
not visible (Fig. 4). Finally, other 97 cases with the hemodynamic pattern
of Type III Shunt and large varicose veins (27%) for cosmetic reasons,
were operated on disconnecting and excising from the LSV all the
incompetent varicose tributaries (Fig. 3). Multiple cosmetic phlebectomy
was also performed (conservative but not hemodynamic treatment). Patients
were discharged 3-5 hours, after surgery with elastic stockings.
Clinical assessment of the results.-The assessment was performed
by an independent assessor who had not been involved in previous surgical
decision making and operative procedure (MGM) according to the following
criteria previously proposed in the literature:
Objective assessment:
- class A: no visible and palpable
varicose veins,
- class B: a few visible and palpable varicose veins
with diameter <5 mm;
- class C: remaining or newly formed varicose
veins with diameter >5 mm;
- class D: insufficient main trunks and
perforator. In addition, functional and cosmetic results were
self-assessed by the patients, at the time of the last examination in
Hospital, using a simple analogue scale well explained by MGM to the
patients themselves:
Subjective assessment:
- class A: no inconvenience;
-
class B: slight functional or cosmetic imperfection, but satisfaction with
the result;
- class C: appreciable functional or cosmetic failure;
improvement but dissatisfaction with the result;
- class D: unaltered
or increased inconvenience.
The four classes, both subjectively and objectively assessed, were
divided in accord with the preoperative hemodynamic pattern (Shunt I or
III) and cesced for significance by the x2 test.
Selection criteria adopted in a sub-group of patients.-After 4
years of mean follow-up we selected other 27 patients for the so called
CHIVA in 2 steps treatment, proposed to avoid treatment failures chat both
the first part of the present study and the literature had shown to
coincide with the hemodynamic patterns of Type III Shunt. In this way a
sub-group of patients affected by superficial incompetence of all stages,
not previously treated, was selected according to the following
ultrasonographic criteria:
Varices supplied by SFJ reflux with re-entry
perforator located in a TV (Type III Shunt). Competent deep venous system.
We selected 27 patients, 22 women and 5 men, mean age 44 years old
(range 24 to 54 years). They also underwent preoperative LSV diameter
assessment at mid thigh, repeated 6 months post-operatively.
CEAP classification.-Patients were prospectively classified in
accord with CEAP. The clinical class, C, ranged to C2 to C5 (12 C2, 10 C3.
4 C4, 1 C5) and all the patients were symptomatic. The etiology, E, was
primary. The anatomical distribution of cases, A, was in the LSV above the
knee in 9 cases, above and below the knee in 18 cases; perforators were
always incompetent at the leg. Finally the pachophysiology, P, was due to
reflux in all cases. The following algorithm describes the selected
patients C2-5, Ep, As2-3 p 18. Pr.
Preoperative duplex mapping.-In all the selected patients duplex
examination allowed the identification of the superficial branch of the PC
represented by the LSV from its junction to the origin of the TV on which
the outlet of the re-entry PV is located (Fig. 5).
Operations.-The treatment is performed in two steps. The first
step is represented by the disconnection of the origin of the TV
containing the "reentry" PV from the main trunk of the LSV, thus
transforming the refluent LSV into an LSV with a forward flow during
muscular contraction, but no Doppler-detectable reverse flow during
muscular relaxation (Fig. 5). However, Doppler-detectable reverse flow
could be demonstrated under Valsalva manoeuvre. The second step,
represented by the section-ligature of the SFJ, is performed when the LSV
again shows a reverse flow due to the development of a new re-entry PV
situated on the LSV itself (transformation into a Shunt type 1) or on a
new insufficient TV.
| Table I.-Pre and postoperative venous
funcion assessment |
| Parameters |
Preoperative |
Postoperative |
Student's "t" and Wilcoxon
tests |
| EV-SFJ |
| AVP |
31.78±4.74 |
20.96±3.24 |
p<0.001 |
| LRR/RT |
12.50±5.18 |
23.68±4.20 |
p<0.001 |
| CHIVA 1 |
| AVP |
50.13±6.56 |
28.82±7.14 |
p<0.001 |
| LRR/RT |
10.12±2.61 |
19.80±4.91 |
p<0.001 |
| Table II.- Results of EV-SFJ (mean
follow-up 52 months) |
| EV-SFJ |
N total |
% |
| Varicose vein recurrences |
7/62 |
11 |
| Long saphenous vein patency |
58/62 |
94 |
| early postop. thrombosis |
2/64 |
3.1 |
| late occlusion |
2/62 |
3 |
| Sapheno-femoral reflux
recurrence |
6/62 |
10 |
| New regurgitations points |
8/62 |
13 |
| Graft infections |
0/62 |
0 |
| Table III. - Results in
CHIVA 1 group/mean follow-up 72 months. |
| Parameters |
Type I Shunt |
Type III Shunt with
re-entry |
Type III Shunt without
re-entry |
Type III Shunt "short or
deep" |
Total % |
| N/total |
% |
N/total |
% |
N/total |
% |
N/total |
% |
Total % |
| Varicose veins disapprarance |
172/186 |
92 |
16/27 |
59 |
81/92 |
87 |
32/35 |
91 |
89 |
| Varicose veins reduction with
exercise |
9/186 |
5 |
8/27 |
30 |
4/92 |
4 |
2/35 |
6 |
- |
| Recurrent reflux site:
Sapheno-femoral |
2/186 |
1 |
1/27 |
4 |
3/92 |
3 |
1/35 |
3 |
2 |
| Perforators |
6/186 |
3 |
1/27 |
4 |
6/92 |
7 |
1/35 |
3 |
4 |
| Sapheno-tributar |
6/186 |
3 |
27/27 |
100 |
2/92 |
2 |
3/35 |
9 |
11 |
| Saphenous vein patency |
184/186 |
99 |
27/27 |
100 |
74/92 |
80 |
35/35 |
100 |
94 |
| Saphenous vein thrombosis |
2/186 |
1 |
0/27 |
0 |
18/92 |
20 |
0/35 |
0 |
6 |
| Symptoms improvement |
183/186 |
98 |
27/27 |
100 |
84/92 |
91 |
35/35 |
100 |
97 |
| Subject Eval |
| Class A |
162/186 |
87 |
8/27 |
30 |
74/92 |
80 |
30/35 |
86 |
81 |
| Class B |
21/186 |
11 |
16/27 |
59 |
14/92 |
15 |
3/35 |
9 |
16 |
| Class C |
21/186 |
1 |
2/27 |
7 |
3/92 |
3 |
2/35 |
6 |
3 |
| Class D |
1/186 |
1 |
1/27 |
4 |
2/92 |
2 |
0/35 |
0 |
1 |
| Object Eval |
| Class A |
172/186 |
92 |
16/27 |
59 |
81/92 |
87 |
32/35 |
91 |
89 |
| Class B |
4/186 |
2 |
3/27 |
11 |
5/92 |
1 |
4/35 |
11 |
5 |
| Class C |
6/186 |
3 |
7/27 |
26 |
3/92 |
1 |
1/35 |
3 |
4 |
| Class D |
2/186 |
1 |
1/27 |
4 |
3/92 |
1 |
0/35 |
0 |
2 |
| Table IV.-Results in two steps CHIVA
group: mean follow-up 18 months |
| Type III Shunt |
N cases |
Rate (%) |
| Varicose vein disappeareance |
27/27 |
100 |
| S-F reflux
disappeareance: |
| Postop |
27/27 |
100 |
| 3 months |
9/27 |
33 |
| 6 months |
19/27 |
70 |
| >12 months |
4/27 |
15 |
| Site of the new
re-entry: |
| Saphenous vein |
10/27 |
37 |
| Tributaries |
13/27 |
48 |
| Neither reflux nor re-entry |
4/27 |
15 |
| Saphenous vein patency |
27/27 |
100 |
| Saphenous vein thrombosis |
0/27 |
0 |
| Symptoms improvement |
26/27 |
96 |
Results
Of the 421 selected patients who entered the study 2 of the EV-SFJ and
17 of the CHIVA group did not finish it. We have divided the results
evaluation into three sections.
EV-SFJ
For these 62 patients follow-up lasted 52 months, ranging from 12 to
84. The outcome evaluation consisted of clinical and duplex scanning
examinations for all the patients every 3 months for the First three years
and then every year. 12 patients underwent descending and 4 ascending
venography. Clinical results are summarized in Table 1. In the early
postoperative period we had 2 saphenous thrombophlebites due to a
technical error, requiring emergency short stripping. Both cases had been
operated on with the hand sewn technique above described and were lost for
further follow-up. All patients were discharged at the day of surgery.
Total varices recurrence race was 12% (7/60). Ultrasonographic follow-up
showed the long saphenous vein completely preserved in 58 cases (94%).
Mean preoperative diameter at middle thigh was 5.6 mm versus 4 mm recorded
after surgery.
Venous function assessment.-AVP and LRR/RT measurements were
performed in 32 cases preoperatively and 6 months postoperatively. AVP and
LRR/RT modifications after surgery evaluated both by Student's "t" and
Wilcoxon tests, demonstrated a highly significant variation (p<0.001)).
(Table II).
CHIVA 1
In this patients' group the mean follow-up lasted 49 months, ranging
from 72 to 12. Clinical and duplex evaluations were made every 6 months
for the first 3 years and then every year. Operations were well tolerated
under local anesthesia. Postoperative analgesic administration was not
necessary. Patients resumed working activity within 3-7 days after
surgery.
Ultrasonographic findings and clinical correlation.-Results are
summarized in Table III, dividing the cases into four sub-groups, Type I
Shunt (186 cases. Fig. 1), Type III Shunt operated on maintaining the
reverse flow from the LSV to a long and superficial TV containing the
re-entry PV(27 cases, Type III Shunt with re-entry in Table III, Fig. 2);
Shunt III operated on without preserving the LSV drainage function (92
cases, Type III Shunt without re-encry in Table III, Fig. 3) and finally,
Type III Shunt with a short or deep TV containing the reentry PV (35
cases, Type III Shunt short or deep in Table III, Fig. 4). Overall
saphenous vein patency recorded was 94%, with a mean diameter measured at
mid thigh of 4.6 mm as compared to 6.2 mm recorded preoperatively. When
patency was demonstrated the saphenous flow was reversed and with low
velocity. Two patent segments of LSV were demonstrated in 29 cases of the
31 LSV interrupted (94%), whereas in 2 cases we ligated the main trunk
above the re-entry perforator causing a symptomatic LSV thrombosis for
technical error. Total recurrences/residual varicose veins registered were
11%, 8% for Shunt I and 16 % for Shunt III, respectively. Symptoms
improved in 97% of cases, no-ulcer recurrences were observed in the
outcome of the 19 patients in pre-operative clinical class 5 or 6.
Subjective and objective assessment of the results.- These
results are also summarized in Table III. Better results obtained with
this technique in patients with Type I Shunt as compared to those
objectively and subjectively assessed in Type III Shunt are statistically
significant (x2=22.144, p<0.0001). However, overall evaluation of the
technique demonstrated 84% of patients in class A, 11% in class B, 4% in
class C and 1% in D (x2 p<0.0001),
Hemodynamic results.-AVP and LRR/RT postoperative evaluations
were done 6 months after surgery. The difference between pre and
postoperative measurements was statistically significant using both
Student's "t" and Wilcoxon's tests (p<0.001), (Table 1).
CHIVA in two steps/or Type III Shunt
The last group of 27 patients with Type III Shunt was operated on using
the two steps CHIVA strategy (Figs. 5, 7). Although the SFJ is not treated
in the first operation LSV reflux and symptomatology disappeared
immediately after. When a new re-entry point-was developed LSV reflux was
newly detected and symptoms worsened. This occurred in 33% of cases after
3 months, in 70% after 6 but in 15°/o of cases after 12/18 months
follow-up neither reflux nor re-entry was detected. The new re-entry
perforator was detected in the LSV main trunk in 37% of cases (Type III
Shunt transformed in Type 1 Shunt) and in 48% newly in a TV, but deep,
short or still not varicose and visible (Shunt type III transformed in
Type III Shunt short and/or deep). The follow-up lasted on average 18
months, ranging from 14 to 24. Clinical and ultrasonographic evaluations
were made every 3 months.
Poscoperative course was quite similar to
that described in the first group. Results are summarized in Table IV.
Discussion
Long saphenous vein sparing surgical procedures have two main
end-points: to perform an ambulatory and effective varicose veins
treatment and to save the long saphenous vein for an eventual future
grafting. This paper also introduces the concept of differentiating the
surgical treatment on the basis of the ultrasonographic features of
patients with varicose veins. We will discuss these three concepts in
regard to the two operations evaluated.
EV-SFJ
Edwards and other authors showed that in early varicose stages valve
incompetence is due to a parietal dilatation with normal valve leaflets.
Hallberg and other authors showed the effectiveness of the external valve
repair both in the deep and in the superficial venous system when this
early pathologic condition has been identified. Current duplex scanning
images can demonstrate the presence of mobile valve flaps at the
sapheno-femoral junction. This examination is crucial in order to plan
external surgical repair.
On the other hand, the present series
suggests a low rate of SFI with high resolution B-Mode evidence of mobile
and of uniform length valve leaflets, thus suitable for the proposed
operation (64/421-15%). These series, with a long follow-up, demonstrate
the effectiveness of this treatment when the proposed indications are
observed. Sapheno-femoral recurrences are fewer than those described in
literature after high ligation, although this is a verv carefully selected
group, all with mild severity of the disease (clinical class 2 according
to CEAP criterial) and thus not comparable with those previously
reported.
In addition, another advantage with respect to high ligation
is the reported higher rate of patent long saphenous veins suitable for
vascular bypasses.
Schanzer comparing in a randomized study high
ligalion-avulsion versus external valve-plasty-avulsion found no
differences in terms of recurrences but a significant difference in LSV
patency race. The present study shows 94% of long saphenous veins
preserved with a mean diameter of 4 mm at the thigh, highly suitable as an
arterial conduit. Furthermore the Veno-cuff device allows an easy and
rapid procedure and its calibrator permits competence control before
firing. We would also underline the absence of prostheses infection in the
outcome. Reliability of CW Doppler for intraoperative assessment of valve
competence was confirmed by intraoperacive angioscopy. Finally, it could
be questionable to assess the SFJ competence in the outcome by the
combination of duplex with the squeezing manoeuver. We showed above and in
Figure 5 that when a varicose network with the hemodynamic pattern of Type
III Shunt occurs, the simple disconnection-avulsion of the LSV tributary
containing the re-entry PV is able to abolish the reflux signal in the
saphenous vein without any additional treatment of the SFJ. Reflux in such
a case can also be detected by means of duplex under Valsalva, and we
recommend adding such a manoeuvre in the outcome evaluation of this group
of patients.
CHIVA
We consider the application of CHIVA in patients with the outlet of the
re-entry perforator on the LSV (Shunt I) to he successful in our long term
follow-up (Table III): 92% of disappearance of varicose veins, 99% of
saphenous vein patency and when the functional and cosmetic results were
subjectively and objectively assessed, we registered excellent and good
results (Class A and B of the scale) in 98% and 94% of the cases,
respectively. This finding is not surprising and previous clinical reports
of CHIVA technique showed satisfactory results for Type I Shunt but
disappointing cosmetic results for persistent or recurrent varicose veins
in the Type III Shunt, the Achille's heel of the CHIVA theory.
Such a
situation is well apparent also in the present study, as comparing the
results registered in Type I Shunt sub-group with that named, in Table
III, as Type III Shunt with re-entry. In the latter the application of the
original CHIVA technique maintains a reflux between the LSV and the TV
containing the re-entry PV (Fig. 2). The varicose tributary, even if
decreased in size, can often be visible after the operation, especially if
dilated, long and superficial. Although this technique allowed appreciable
functional results, the negative impact in subjective and objective
assessment of cosmetic results in this sub-group of patients is well
apparent in Table III. Conversely, in 35 patients with the hemodynamic
pattern of Type III Shunt, and a deep or very short segment of the
tributary between the LSV and the re-entry perforator, functional and
cosmetic results were not significantly different from that obtained in
the Shunt I (Table III). It is intuitive that the depth or the shortness
of the insufficient tributary in these cases assures an acceptable
cosmetic result (Fig. 4), Finally in other 92 patients with the
hemodynamic pattern of Type III Shunt we treated the patients with flush
ligation plus disconnection and avulsion of the varicose tributaries, in
order to avoid the above mentioned cosmetic problems (Fig. 3). Such a
treatment can be assimilated to the classic conservative but not
hemodynamic treatment described in the literature, planned on the basis of
careful pre-operative duplex mapping. The graded responses for symptomatic
and cosmetic outcome were classified as successful for patients in class A
and B, and, according to this classification the subjective and objective
outcome was judged to be successful in 89% and 88% of cases,
respectively.
Fligelstone using the same procedure after four years
follow-up reported a successful subjective and objective outcome in 84%
and 87% of cases, respectively and the group of Hammarsten in Sweden a
successful subjective outcome in 94% of cases following the same surgical
procedure. In the latter such a result was not significantly different
from that assessed using stripping in the contralateral limb. As far as
LSV patency is concerned, only when the re-entry PV is preserved we are
capable of detecting by means of duplex a flow in LSV (Figs. 1. 2. 4). The
data analysis of Table III well demonstrates this finding: -In Type I
Shunt, 2 cases of LSV occlusion were due to the incorrect ligation of the
saphenous trunk above the PV. In 31 cases we ligated the LSV below the PV
and we preserved at least two long and patent segments of LSV, suitable
for eventual grafting. In 153/186 cases we preserved a patent LSV for its
whole length. -When Type III Shunt, was operated on maintaining the
re-entry PV the LSV was found to be patent in 100% of cases (sub-groups
Type III Shuni with re-entry and Type III Shunt shon or deep in Table
III).
-Non-draining and occluded LSV were found in 20% of the cases
operated without planning a reentry for the reverse saphenous flow
(sub-group Type III Shunt without re-entry in Table III). Moreover,
previous reports demonstrate CHIVA effectiveness, when the draining
function of the saphenous vein is maintained. Non-draining saphenous vein
presented in the outcome a higher rate of recurrences in addition to its
obvious unsuitability as arterial conduit. In the present study, the Type
I Shunt group presented 99% LSV patency and 92% varicose veins
disappearance, whereas in Type III Shunt we registered a race of 88% and
84%, respectively (p<0.001).
Refluent LSVs present during muscular
contraction a forward flow due to the action of the muscular pump, and
during muscular relaxation a reverse flow directed towards re-entry PVs
(Fig. 5a). SFJ closure causes the disappearance of the forward flow but
does not interfere with the reverse flow (Fig. 7). On the other side, the
ligation of the re-entry PV, or of the origin of the TV which contains it,
causes the disappearance of the reverse flow but does not incerfere with
the forward flow, which remains preserved (Fig. 6). In both cases the LSV
is able to empty. In contrast, when reflux and re-entry points are
suppressed at the same time, no Doppler-detectable flow is present, and
thus the LSV becomes a "non-draining" vessel.
For this reason, we were
surprised when Campanello reported a 100% saphenous vein patency in the
outcome of high ligation and distal avulsion with meticulous ligalion of
all incompetent perforators, localized by means of preoperative
venography. This result is highly questionable since the saphenous trunk
does not have any more a possibility- of emptying. Following high ligation
and multiple avulsions. Rutherford reported a 21% rate of saphenous
occlusion and Fligelstone only a 64% of patent and suitable LSV for bypass
surgery. Finally, based on such hemodynamic considerations and on the
results of CHIVA treatment of Type III Shunt a new technique, named CHIVA
in two steps, was proposed. The first step is represented by the
disconnection of the origin of the TV containing the re-entry PV, thus
transforming the refluent LSV into a LSV with a forward How during
muscular contraction, but no Doppler-detectable reverse flow during
muscular relaxation (Fig. 5). The second step. represented by the
section-ligature of the SFJ, can be performed when the LSV again shows a
reflux due to the development of a new re-entry represented by a PV
situated on the LSV or again, on a TV (Fig. 7). Based on the above
mentioned results, when reflux re-appears with the hemodyna'mic patterns
of type I Shunt or of Type III Shunt with short or deep re-entry (Figs. 2,
3) the second step was represented by simple high ligation (Fig. 7). This
tactic was performed in 85% of cases with successful functional and
cosmetic results (Table IV), even if with a very short and thus still
inconclusive follow-up. We would like to underline in 15% of cases the
absence of a detectable reverse flow after 12 - 18 months follow-up from
the first procedure. Moreover, until now we never observed the development
of an incompetent TV long and superficial. analogue to that avulsed with
the First procedure. However, a larger number of treated cases and a long
term follow-up is required in order to evaluate the possible role of CHIVA
in two steps in varicose vein treatment sparing the saphenous vein.
Conclusions
Long saphenous vein sparing surgical procedure alternatives to high
ligation and distal stab avulsion seem to be advantageous for future
grafting because a higher rate of long saphenous vein paiencv was found.
All the illustrated techniques suppress reflux while maintaining a
saphenous flow. Following CHIVA I and the second step of CHIVA 2
procedures the LSV drains blood with a reverse flow toward the re-entry
PV, whereas after EV-SFJ and the first step of CHIVA 2 with the
physiological flow through the junction. Further studies are warranted in
order to verify the association between draining and patent LSV and
successful outcome of varicose vein treatment on one hand, and with the
suitability of the vein for arterial reconstruction






