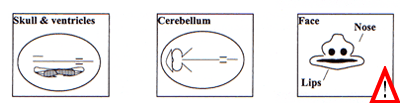
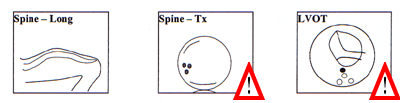
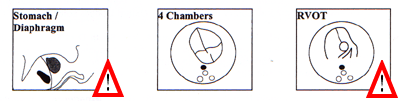
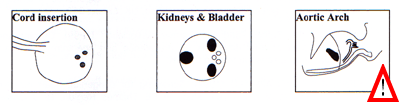
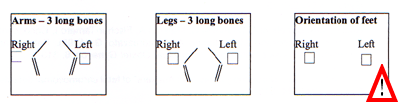
Scorrendo la pagina verso il fondo potete anche trovare delle figure (Appendice 1) che illustrano le strutture anatomiche fetali da esaminare in una ecografia ottimale ("optimal scan" come è chiamata in queste linee guida). Vi ho contrassegnato con un segnale di punto esclamativo le strutture che non sono comprese nelle linee guida italiane.
| Ultrasound
Screening
July 2000 Supplement to Ultrasound Screening for Fetal Abnormalities CONTENTS Membership of the Working Party 1. Introduction Appendix 1 Baseline fetal anomaly scan MEMBERSHIP OF THE WORKING PARTY Professor M J Whittle FRCOG (Chair) Dr L S Chitty MRCOG Professor J P Neilson FRCOG Dr I M Shirley FRCR Dr N C Smith FRCOG Professor Y G Ville MD Mr M P Wyldes MRCOG Acknowledgments Dr P Chudleigh Professor T Marteau Professor K Nicolaides Professor C Rodeck Dr S Russell Professor P Soothill Royal College of Radiologists National Screening Committee 1. INTRODUCTION The 1997 Report of the Royal College of Obstetricians and Gynaecologists Working Party on Ultrasound Screening for Fetal Abnormalities(1) identified that one of the problems with screening scans was the variable way in which they were conducted throughout the country. There are no clear guidelines about what should, or should not, be examined. Sonographers are trained to look at all structures; however local resources, such as the quality of ultrasound equipment and the time available for each examination, may dictate exactly what is examined, certain structures being more readily sought than others. As a result there can be a lack of clarity about the content of the examination which can lead to confusion for both ultrasonographer and patient. A supplementary Working Group was convened in 1998 to produce a standard format for a 20 week anomaly screening scan. The Group agreed that a two-stage ultrasound examination programme was acceptable, and a recent survey (unpublished) from the Joint Committee of the Royal College of Obstetricians and Gynaecologists/Royal College of Radiologists indicates that probably at least three quarters of the units in the country use such a programme. This paper provides recommendations for the two-stage scan programme: an initial scan performed at booking and the second at or around 20 weeks' gestation. The role of anomaly scanning in the later first/early second trimester has not been established although research in this area continues. 2 The Early Pregnancy Scan 2.1 The first scan in early pregnancy, referred to as a booking scan, is undertaken ideally before 15 weeks. The purpose of this scan should be to establish:
Randomised studies(2) suggest that at least one routine scan in pregnancy to confirm gestational age confers benefit, especially in reducing the need for intervention for post-maturity. If serum testing is to be used as a method of screening for Down syndrome, accurate knowledge of gestational age is essential(3). 2.2 The Procedure. Before 13 weeks, gestational age can be accurately assessed from the measurement of crown rump length. However, from 13 weeks crown rump length should not be used because the fetus becomes increasingly flexed making the measurement unreliable. As an alternative bi-parietal diameter, and/or head circumference should be used; some units include femur length measurement. 2.3 The early scan can usually be performed abdominally but, on occasion, a vaginal scan is necessary. 2.4 As far as scanning for nuchal translucency is concerned, current evidence suggests that this is an effective way of determining babies at risk of Down syndrome and is best performed between 10-14 weeks. Whether it is preferable to serum testing remains to be decided and it is most likely that a combination of serum testing and nuchal translucency measurement will produce the highest sensitivity for the lowest false positive rate. However, whether or not nuchal translucency screening is introduced is a funding issue for individual Trusts. The Department of Health is awaiting the report of the Serum, Urine and Ultrasound Screening Study (SURUSS) before it decides on its position with regard to funding nationally. 3 The "20 week" Anomaly Scan 3.1 In units in which a booking scan is not performed, the "20 week" scan provides dating information and diagnosis of multiple pregnancy. The majority of non-viable pregnancies will be lost before the scan at twenty weeks. 3.2 The twenty week anomaly scan is to reassure the woman that her baby appears to have no obvious structural abnormalities. Lack of explicitness about which structures have been examined may lead to confusion. The literature provides a range of detection rates and therefore individual units should provide their own figures to inform women undergoing the "20 week" scan. Recent data(4) from one unit would suggest that about 50% of significant abnormalities will be identified by a screening scan. The value of identifying fetal abnormalities at this stage is that it offers parents options. Some, probably the majority, for serious lesions, will elect to terminate the pregnancy. Those couples who choose to continue the pregnancy have the opportunity to prepare themselves through discussions with health care personnel and self-help groups, whilst attendants can ensure appropriate care during pregnancy and following delivery. 3.3 The objectives of the ultrasound examination should be made as explicit as possible to women and their partners to enable them to opt for, or opt out of, having a scan. For example, women who do not wish to be informed of a risk of aneuploidy may consider not having a scan at all. 3.4 A national standard for a routine ultrasound anomaly scan is recommended by the Working Group. This would provide parameters for sonographers, choice of options for women and provide purchasers with indications of how much screening could be accomplished within the available resources. For example, an individual Trust could make a clear decision that it does not have the resources for ultrasonographers to examine cardiac outflow tracts. A clear indication of what could, and what could not, be achieved with screening will remove a wide area of uncertainty and would alleviate anxieties for both women and sonographers. 3.5 The Working Group propose that a "20 week" scan should be to a minimum standard, which should be made clear to the woman in the form of a leaflet. If a unit considers it cannot deliver scans to this minimum standard then the "20 week" scan should be abandoned. Under these circumstances the woman should have a single scan in pregnancy to establish the objectives outlined in paragraph 2.1. If the equivalent of a "20 week" scan is desired the woman should be referred to an appropriate unit. 3.6 The Procedure 3.6.1 The minimum standard for a "20 week" anomaly scan Gestational age can be established by measurement of bi-parietal diameter, head circumference and femur length. The inclusion of abdominal circumference would be optional. Fetal Normality
3.6.2 The optimal standard for the "20 week" anomaly scan If resources allow, the following could be added to the features in 3.6.1:
It is likely that the "optimal scan" will only improve the detection of cardiac abnormalities and clefts. Recent evidence(5) seems to demonstrate above average detection of fetal cardiac abnormality in areas which have most likely been influenced by a training programme for ultrasonographers started at Guy's Hospital some years ago(6). However, ensuring the outflow tracts are intact takes additional time and may require the woman to return for a further check in 15% of cases; an additional 9% may need another review(7). 3.7 A checklist for the baseline fetal anomaly scan is included as Appendix 1. 3.8 Guidance on screening for aneuploidy for the professional is included in Appendix 2. 3.9 Markers 4. Standards 4.1 Quality of information given to patients, and its
explicitness 4.2 Setting and timing 4.2.1 The ultrasound examination should be undertaken in an area/room designed for the purpose. About 20 minutes should be allocated for the whole investigation including introduction and documentation. 4.3 Care and support for women undergoing screening 4.3.1 Every department undertaking screening scans should have at least one individual trained in counselling in the area of prenatal diagnosis and screening. 4.3.2 Wherever screening for fetal abnormalities is undertaken, it should be possible for the woman to discuss issues about screening with a named midwife/counsellor with particular interest/expertise in the area. 4.3.3 A quiet room should be available for the use of the trained counsellor to talk to women who need to receive and understand bad or troublesome news about their baby. 4.3.4 Discussion of the implications of a suspicious scan should occur with an obstetrician within 24 hours (or one working day). If indicated, referral to a tertiary centre with maternal fetal medicine specialists and other relevant practitioners should be possible within 72 hours (or two working days). If referral to a tertiary centre is not possible within this time limit then at least an explanation about the need for referral should be given. 4.3.5 Women should receive written details about their scan result and, whenever possible, information concerning the type of fetal abnormality present. 4.3.6 There should be a mechanism in existence whereby the woman with an abnormal scan can be followed up and supported. 4.4 Record keeping 4.4.1 All scans should be carefully documented and archived. The use of hard copy for routine normal scans has major cost implications. However when abnormalities are found, or when specific structures are seen which may appear suspicious, hard copy or preferably video recordings are recommended. 4.4.2 Accurate record keeping is needed to ensure that pregnancy outcome is recorded with sufficient detail to ensure that feedback is comprehensive. 4.4.3 Depending on workload, the employment of appropriate support staff/clerks to maintain high standards of record-keeping is recommended. 4.5 Computer-based records. 4.6 Quality and Audit 4.6.1 Every unit should audit its results with respect to the detection of fetal abnormalities on an annual basis. The results of the audit should be included in the information provided to women, for example in a patient information leaflet. 4.6.2 A high standard of perinatal pathology with feedback to the ultrasound department is an essential element of a screening service. The continual monitoring of results in terms of accuracy of diagnosis is mandatory. 5 Assessment of screening programmes The monitoring of the screening process and its ability to pick up abnormalities can only be achieved through regional anomaly registers. The following issues are important:
6 Training 6.1 Sonography is not recognised as a specialty by the Health Act 1999, so there is no obligation for sonographers to be registered to practise. There is currently no statutory requirement for ultrasound practitioners to receive accredited training. 6.2 Many sonographers will have achieved a postgraduate certificate or diploma in clinical ultrasound. Well-established programmes leading to these qualifications are available in a number of universities in the United Kingdom and the courses are accredited by the Consortium for the Accreditation of Sonographic Education (CASE). Members of the consortium include the British Medical Ultrasound Society, the College of Radiographers, the Royal College of Midwives and the United Kingdom Association of Sonographers. 6.3 To achieve and attain CASE accreditation an individual course must demonstrate that both its academic and clinical teaching programmes and its assessment methods are sufficiently rigorous to ensure that successful students are safe to practise in the ultrasound areas for which they have studied. Current postgraduate education certificates/diploma training programmes in obstetric ultrasound are designed with the provision of a safe, accurate and efficient screening service for fetal abnormality in mind. 6.4 There is a need for practical competence tests at Trust level. The Working Group recommends that local departments monitor standards and keep checks on them. 6.5 Trusts should have a process for retraining and updating as required but at present there is little provision for this in Trust budgets. Clinical governance provides a facilitating mechanism. 6.6 Medical staff who undertake ultrasound scanning for fetal abnormalities should ideally, and increasingly, hold the Advanced Certificate of Ultrasound Training which is issued following a 300 hour course held in centres recognised by the RCOG/RCR. Skills should be maintained by performing detailed scans in at least one and preferably two sessions a week. 6.7 Medical staff should not undertake scans of any sort if they have not been specifically trained. 7 Equipment 7.1 A scan to perform a fetal structural survey demands the use of modern equipment (not more than 5 years old) of modest sophistication. The scanner must be capable of performing the necessary measurements and should provide good image quality. As always, regard for safety in the use of ultrasound is paramount and minimum output should be used in accordance with the ALARA principle - As Low As Reasonably Attainable. 8 References
Appendix 1 Baseline fetal anomaly scan Extended views
Appendix 2
Ultrasound for Screening for Aneuploidy
Guidance for the professional If you are scanning at 20 weeks it is very important to know
what screening has already been undertaken in your population. If
your population has already been screened using maternal age
alone, or in combination with nuchal translucency measurement or
serum screening, 50-80% of affected cases will already have been
identified, and it is therefore much less likely that a
sonographic marker will be linked to aneuploidy, most typically
trisomy 21, than in an unscreened population.
Ultrasound Checklist
Sonographic "markers" for aneuploidy Other risk
factors Appendix 3
Your Ultrasound Scan As part of your antenatal care we are offering to do a scan of
your pregnancy.
The first scan will be done at your antenatal visit. It is to
check how many weeks pregnant you are, that there are not twins
and that the baby is doing well. Usually the scan will be through
your abdomen and you should have a full bladder. Sometimes the
scan will be done through the front passage (vagina) but the
ultrasonographer will talk to you about this if it proves
necessary.
A second scan, done at about 20 weeks, is to check that your
baby is normal. Most babies are healthy, but sadly some have
problems which could be serious. If you really do not wish to know
if the baby has an abnormality, it may be best to decide not to
have this scan. If you do decide to have a scan we will assume
that you wish to know about anything that we find.
The scan will involve you lying down on a couch, and a trained
scan operator putting scan gel and then the scan head onto your
abdomen. This will give images on the screen which allow
measurements of the baby and give moving pictures. These can be
quite difficult to see clearly, but the scan operator will try to
ensure that all is well.
About half of the major abnormalities which cause serious
difficulties will be seen on a scan and half will not be
seen. This means that even if your scan is normal there is a small
chance that your baby will still have a problem.
Below is a list of different types of congenital abnormality,
and how likely scanning is to identify each problem.
The scan can sometimes tell what sex the baby appears to be,
but not always, and we would usually not do extra scans just to
identify the sex of the baby. If the scan does predict the sex of
the baby this is right about 95% of the time. The scan operator
will only tell you the sex of the baby if you, and all the people
in the scan room with you, want to know that information.
If the scan finds a problem you will be told at the time of the
scan that there is a problem, but a full discussion of the problem
may require you to come back to the hospital for a further scan
and discussion with a specialist. Most problems that need repeat
scanning are not serious and approximately 15% of scans will need
to be repeated for one reason or another.
APPENDIX 4
Potential Detection Rates based on Screening Strategy(9)
A six year study in Scotland Booking Scan Minimum
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||